Hospitals and clinics are busy, complex places. Behind every clean hallway and safe patient room, there’s a network of systems and people making sure the environment stays healthy and risk-free. That’s where EHS, or Environmental Health and Safety, comes in. In healthcare, EHS isn’t just about compliance or checklists – it’s about protecting patients, staff, and visitors from harm. From managing hazardous waste to controlling infection risks, EHS teams quietly keep the entire operation running safely in the background.
What “EHS” Stands For – A Quick Refresher
EHS stands for Environment, Health, and Safety – three areas that, together, form the foundation of how organizations keep people safe and operations responsible. In simple terms, EHS is about preventing harm before it happens. It’s the framework that guides how companies handle chemicals, manage waste, protect workers, and maintain safe environments for everyone involved.
In healthcare, though, this idea goes far beyond the basics. A hospital isn’t like a warehouse or an office building. Every corner of it carries potential risks – from radiation in imaging departments to biohazardous waste in labs, from disinfectant fumes in cleaning closets to sharp instruments in operating rooms. Even something as small as a misplaced chemical container or an unventilated storage area can cause real problems.
Examples of EHS in Healthcare
- Managing chemical and biological waste safely
- Monitoring air quality, water systems, and indoor ventilation
- Ensuring staff use proper protective equipment
- Conducting safety audits and emergency drills
- Training employees to recognize and report hazards
- Keeping facilities compliant with environmental and occupational safety laws
EHS in healthcare brings all these moving parts under one system. It ensures the air is clean, the waste is handled safely, and the people who work there have the right protection and training. It also helps hospitals stay compliant with strict environmental and safety laws, which is no small task. The ultimate goal isn’t just to avoid accidents or penalties – it’s to create a culture where patients, staff, and visitors can feel safe the moment they walk through the door.
Why EHS Is Especially Critical in Healthcare
When you walk into a hospital, you don’t just see doctors and patients – you see an entire ecosystem working together. Labs filled with chemicals, radiology rooms with high-energy equipment, emergency wards that never sleep, and cleaning teams handling infectious waste around the clock. Each area has its own risks, and without a strong EHS program, those risks can quickly add up. That’s why environmental health and safety isn’t just a “nice to have” in healthcare. It’s something that keeps the entire system stable, safe, and functional.
Why EHS Matters in Healthcare
Patient and staff safety
The most obvious reason EHS matters is that it protects people. Hospitals handle sharp instruments, biological waste, radiation, and strong cleaning agents daily. If even one of those is mishandled, someone could get seriously hurt or sick. EHS helps set up procedures and training so staff know how to store chemicals, dispose of waste, and respond to incidents. It’s what keeps small mistakes from turning into major problems.
Regulatory compliance
The healthcare industry operates under strict rules for a reason. There are federal and local laws that govern how waste is treated, how air is filtered, and even how certain rooms must be built. EHS programs help hospitals stay compliant by monitoring practices, maintaining records, and ensuring inspections go smoothly. It’s not just about avoiding fines – it’s about proving to patients and regulators that safety is a core value, not an afterthought.
Operational continuity
A single safety incident can disrupt an entire hospital unit. A chemical spill in a lab might shut it down for days, or an outbreak of infection could limit patient capacity. EHS teams work to prevent that by identifying risks early, enforcing preventive maintenance, and making sure every department has an emergency plan. In a place where every minute counts, these safeguards keep care running smoothly.
Culture of safety
Good EHS programs do more than enforce rules – they help build a mindset. When staff know their safety is prioritized, they’re more engaged and attentive. That culture spills over into patient care too. It shifts safety from being a checklist item to being something everyone takes personal responsibility for. Over time, that attitude changes how the whole organization operates.
Environmental responsibility
Hospitals use an enormous amount of energy, water, and materials. They also produce tons of waste, much of it hazardous. EHS programs push healthcare institutions to think beyond the walls of their facilities – to consider their impact on the planet. That can mean improving waste segregation, recycling where possible, or adopting energy-efficient systems. It’s a step toward more sustainable healthcare, which benefits everyone in the long run.
In short, EHS is the quiet backbone of a safe healthcare system. It allows hospitals and clinics to focus on what they do best – caring for people – while knowing that the environment, the staff, and the patients are all protected.
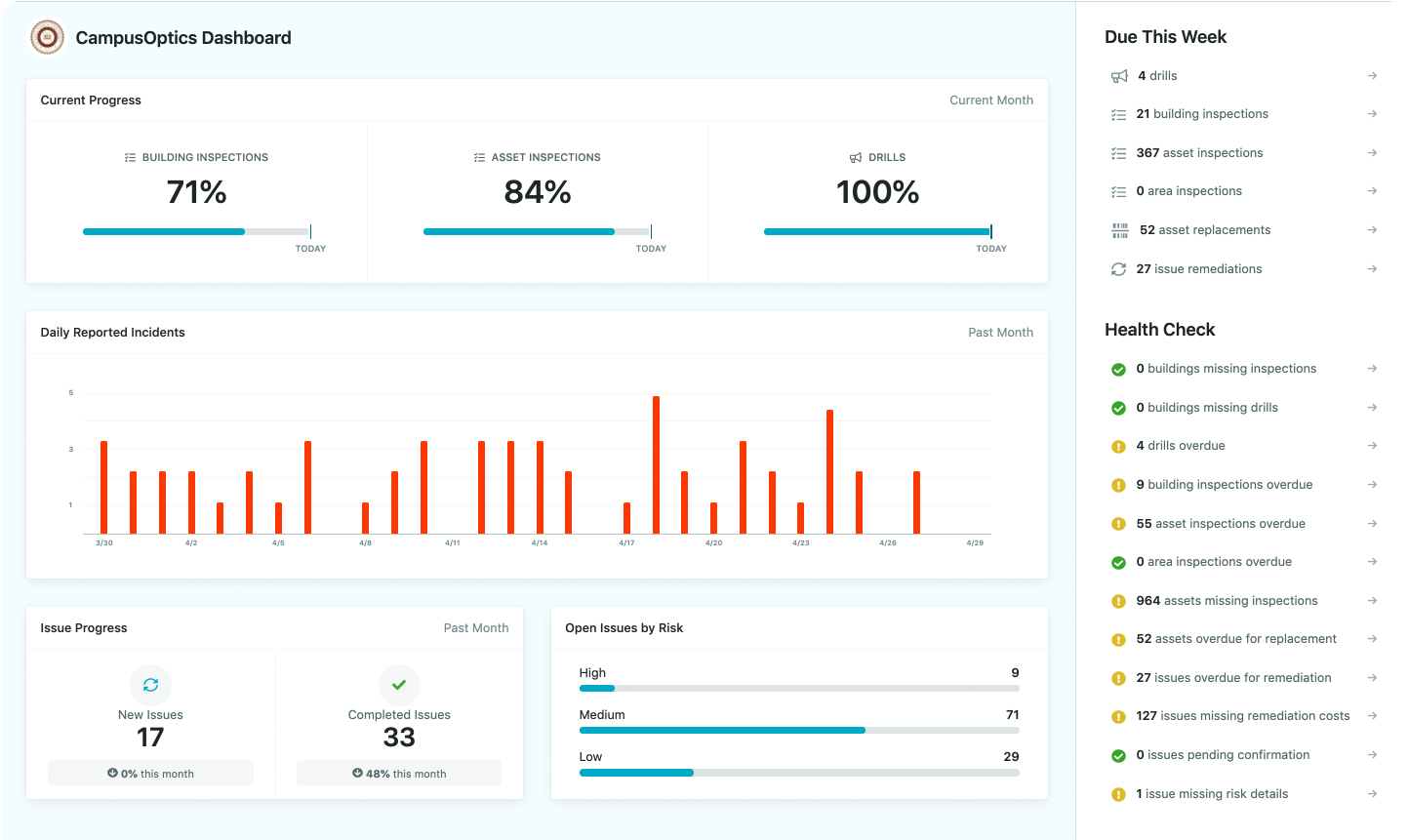
How We See EHS Technology Making a Difference with CampusOptics
Technology has completely changed how Environmental Health and Safety programs work, especially in complex environments like hospitals, universities, and research facilities. Instead of juggling spreadsheets, paper logs, and endless emails, safety teams can now manage everything in one place. That’s where CampusOptics comes in.
At CampusOptics, we’ve seen firsthand how digital tools can simplify even the most complicated EHS tasks. Our platform helps institutions stay ahead of risks by bringing chemical inventory, waste management, safety inspections, and emergency planning into one connected system. Because safety professionals spend most of their time out in the field, we made mobility a core feature – giving them access to everything they need right from their phone. Whether it’s scanning a barcode on a chemical container, logging an incident, or pulling up a safety plan, CampusOptics keeps safety information where it belongs: in the hands of the people who need it most.
For us, technology isn’t just about automation. It’s about helping healthcare and education professionals build stronger safety cultures – ones that protect people, prevent incidents, and make compliance a natural part of daily work rather than a chore.
The Three Pillars in the Healthcare Setting
Let’s break down Environment, Health, Safety – what they each mean in a healthcare facility.
Environment
This refers to external and internal environmental factors – chemical, biological, physical. In hospitals that could mean:
- Safe disposal of hazardous/chemical waste
- Managing emissions or spills
- Controlling contamination of air and water
- Using resources efficiently (energy, water)
- Minimising impact on the surrounding community
Health
In a healthcare facility “health” doesn’t just mean patient health but the health of staff, visitors, contractors. For example:
- Monitoring and protecting staff from radiation, chemical exposure, ergonomic injuries
- Preventing occupational illnesses
- Supporting mental health and fatigue management for staff who work long shifts
- Ensuring patient health isn’t compromised by environmental or safety hazards
Safety
Safety is the more familiar piece: preventing accidents, injuries, unsafe conditions. In healthcare, safety might include:
- Preventing slips/trips/falls in a ward or operating room
- Managing electrical safety, equipment calibration
- Emergency preparedness (fire, active shooter, chemical accident)
- Infection prevention and control
Each of these areas overlaps and feeds into the others–a good EHS programme in a hospital treats them as part of a whole rather than isolated silos.
What “EHS in Healthcare” Looks Like in Practice
So how does this all translate into real operations inside a healthcare institution? Let’s look at some concrete examples.
Hazardous Materials & Waste Management
Hospitals handle a huge variety of materials: chemicals (cleaning, lab reagents), radioactive materials, sharps, biohazardous waste. An EHS programme will ensure:
- Proper inventory and tracking of chemicals and radioactive sources.
- Waste streams are identified, segregated and disposed of according to regulation.
- Staff are trained in safe handling, spill response, disposal.
- Inspections and audits check compliance.
Infection Control and Environmental Safety
Although infection control is often handled by a dedicated team, EHS supports it by ensuring the environment is managed:
- Heating, ventilation, air-filtration systems are maintained.
- Surfaces are cleaned, hazardous areas isolated.
- Protocols exist for cleaning labs and suites where infectious agents are present.
- Monitoring and auditing of environmental cleanliness and safety.
Staff Safety and Occupational Health
In a hospital context:
- Staff might be exposed to radiation, ergonomic stress, chemical exposures, patient violence.
- EHS programmes implement training, PPE, monitoring, incident investigation.
- Regular inspections of equipment, environment and work practices help identify risks before they become incidents.
Emergency Preparedness and Business Continuity
Hospitals must be ready for fires, natural disasters, chemical spills, mass-casualty events. EHS planning covers:
- Emergency pre-plans and drills
- Systems for rapid response and recovery
- Ensuring that patient care areas remain operational in these events
Data, Auditing and Compliance
You can’t manage what you don’t measure. Healthcare EHS programmes typically include:
- Incident reporting systems
- Audit programmes (inspections, compliance checks)
- Training records
- Environmental monitoring (air, water, waste)
- Regulatory tracking
Key Benefits of Strong EHS in Healthcare
When an EHS program is done right, the difference is easy to see – and even easier to feel. It shows up in the day-to-day rhythm of a hospital: smoother operations, calmer staff, fewer emergencies, and a general sense that things just work as they should. These results don’t happen by accident; they come from a system that keeps safety and health at the center of everything.
Benefits of a Strong EHS Program
Fewer incidents and injuries
A strong EHS program helps catch risks before they turn into accidents. Simple things like better labeling, cleaner storage, or regular equipment checks can prevent serious harm. The fewer disruptions there are, the more time staff can spend focusing on patients instead of dealing with injuries or repairs.
Lower regulatory risk
Hospitals and clinics operate under some of the toughest safety and environmental standards out there. An organized EHS system keeps track of inspections, training records, and waste documentation so nothing slips through the cracks. That means fewer compliance issues, fewer fines, and a much smoother relationship with regulators.
Higher staff morale
People feel better about coming to work when they know their safety matters. Having the right protective gear, clear procedures, and responsive leadership reduces stress and builds trust. Over time, that creates a workplace culture where employees feel valued and confident in what they do.
Better patient outcomes
A safe, well-maintained environment isn’t just good for staff – it directly affects patients too. Clean air, properly sterilized equipment, and quick responses to safety issues all contribute to faster recovery times and fewer complications. When EHS is strong, patients benefit in ways they may never even notice.
Real cost savings
It’s not just about safety for safety’s sake. Preventing accidents, reducing waste, and maintaining compliance all save money in the long run. Hospitals can avoid expensive downtime, insurance claims, and legal costs – while keeping resources focused on care rather than damage control.
Improved reputation and community trust
A healthcare facility that consistently demonstrates safety and environmental responsibility earns credibility. Patients, families, and even potential staff see it as a place that takes its duty seriously. That kind of trust doesn’t come from marketing – it’s built through everyday actions that reflect real accountability.
In the end, a strong EHS program doesn’t just prevent problems; it sets the tone for how a hospital operates. It creates a safer, more reliable environment where both people and care can thrive.
Common Challenges in Implementing EHS in Healthcare
Implementing an effective EHS programme in healthcare doesn’t come without hurdles. Some of the more common challenges include:
- Complexity of operations: hospitals are busy, 24/7, with multiple departments, contractors, variable workflows.
- Resource constraints: EHS functions may be understaffed or under-funded in healthcare when compared to industry.
- Cultural barriers: clinical staff may focus on patient care and see EHS as an “administrative” burden rather than an enabler.
- Data silos: environmental, safety and health data may live in separate systems, making it hard to get a unified view.
- Rapid change: healthcare technology, regulatory requirements and patient demographics are all changing fast. Maintaining currency in EHS is demanding.
- Visibility: because EHS is often behind the scenes (meaning “nothing happened today”), its value may be under-recognised.
Steps to Build or Improve an EHS Programme in a Healthcare Setting
Here’s a suggested approach to either get started or mature your EHS efforts in healthcare:
Conduct a baseline risk assessment
- Map out all the major hazard types in your facility (chemical, biological, physical, ergonomic, environmental)
- Prioritise by risk and impact
Define a policy and governance structure
- Establish an EHS policy that aligns with your organisation’s overall mission
- Set roles and responsibilities (EHS professionals, safety committees, department heads)
Develop and implement controls
- For the highest-priority risks, put in place controls (engineering, administrative, PPE)
- Develop standard operating procedures (SOPs), training plans, inspection schedules
Integrate with clinical operations
- Ensure that EHS is embedded in everyday workflows – labs, wards, maintenance, supply chain
- Collaborate with infection control, risk management, facilities management
Use technology and data
- Build dashboards to monitor incidents, training completion, audits
- Leverage mobile tools to enable inspections, issue logging, tracking of corrective actions
Training and culture
- Engage staff at all levels: frontline staff, supervisors, management
- Highlight that safety and environment are part of patient care, not a separate or “extra” task
Continuous improvement and auditing
- Conduct regular audits and inspections
- Analyse incident data for root causes and trends
- Update your risk assessment and controls periodically
- Benchmark performance and report to leadership
Future Trends – What’s Coming Next for EHS in Healthcare
Like many fields, EHS is evolving. In healthcare you’ll see these trends:
- Digital tools and analytics: More use of mobile inspection apps, incident management platforms, dashboards with real-time data.
- IoT and sensors: Air-quality monitors, radiation sensors, asset tracking in real time.
- Integration with patient safety and quality programmes: EHS will increasingly link to clinical quality, infection control and patient experience.
- Sustainability and ESG focus: Healthcare organisations are under pressure to reduce environmental footprints and will tie EHS programmes to broader sustainability goals.
- Culture and human-factors focus: Recognising that technology alone isn’t enough–behaviour, staff engagement and culture matter.
- Regulatory complexity: The regulatory landscape will keep changing; EHS programmes will need to be more agile.
Conclusion
EHS in healthcare isn’t just another layer of policy or paperwork – it’s the framework that quietly keeps everything running safely behind the scenes. It connects the air people breathe, the waste they dispose of, and the way they respond when something goes wrong. When done well, it protects not only patients and staff but the environment that supports them.
The truth is, healthcare doesn’t stop for anyone. It runs 24 hours a day, every single day of the year. That’s why EHS matters so much here. It gives structure to chaos and helps people make smart, safe decisions even in high-pressure situations. Whether it’s keeping track of chemical inventories, preparing for emergencies, or preventing infections, every small EHS task adds up to something much bigger – a culture of care that goes beyond treatment rooms and hospital walls.
As healthcare keeps evolving, the role of EHS will only grow. New technologies, tighter regulations, and rising expectations mean organizations have to stay proactive, not reactive. The goal isn’t perfection, but progress – building safer, more sustainable systems that protect everyone who walks through the door. In the end, that’s what EHS in healthcare is really about: creating places where healing can happen without harm.
Frequently Asked Questions (FAQ)
1. What does EHS mean in healthcare?
EHS stands for Environment, Health, and Safety. It’s basically the framework that helps hospitals and clinics keep people safe while protecting the environment. Think of it as the behind-the-scenes system that makes sure chemicals are stored correctly, waste is handled safely, and staff have the right training to prevent accidents.
2. Why is EHS such a big deal in hospitals?
Because hospitals are full of potential hazards – chemicals, infectious waste, radiation, heavy equipment, you name it. Without clear safety systems, small mistakes can turn into serious problems. EHS programs help catch those issues early and keep both patients and staff out of harm’s way.
3. Who handles EHS in a healthcare facility?
It’s usually a team effort. Most hospitals have an EHS manager or safety officer, but department heads, nurses, lab technicians, and maintenance staff all play a role. Everyone has to do their part for the system to actually work.
4. How does EHS connect to patient care?
You might not notice it, but EHS directly affects how safe and smooth patient care feels. Clean air, proper infection control, well-maintained equipment – all of that falls under EHS. When those pieces are handled properly, patients heal in a safer environment and staff can focus on care instead of putting out fires.
5. How is technology changing EHS in healthcare?
Digital tools have made EHS much easier to manage. Platforms like CampusOptics bring everything into one place – inspections, training, incident reports, and even chemical inventories. It saves time, reduces errors, and helps safety teams stay organized, especially when they’re constantly on the move.
6. Can smaller clinics really afford to implement EHS programs?
They can, and they should. It doesn’t have to be complicated. Starting small with clear safety policies, proper waste disposal, and a few digital tools for recordkeeping can make a big difference. Over time, those small steps build a strong foundation.